I’d like to tell you about my experience of living with Hereditary Angioedema (HAE) and to explain some of the issues that I am facing in trying to be a responsible patient, engaged in my own care. I guess it’s an attempt to improve awareness of the condition whist trying to process my very mixed emotions as tomorrow ,1st August 2013, I’m having my first training session for self administration of Berinert (C1 esterase inhibitor, human) which I am hoping will give me greater control and a better quality of life, hence the title of this blog!
As I explained in my first blog HAE is a rare condition; incidence 1/10,000 to 1/50,000 of the population, caused by a defect in the gene that controls a blood protein called C1 Inhibitor (C1 INH), part of a complex cascade of reactions that control the release of fluids from capillaries into the surrounding tissues, thereby causing oedema (swelling). It is an inherited condition and if a parent has HAE, there is a 50 % chance they will pass it on to their children, and luckily I haven’t! Family members who have been tested and who do not have HAE will not pass the disease on to their children. However , HAE can also occur with no family history as a spontaneous gene mutation, I am one such mutation. Attacks can start at any time from early childhood, in adolescence or later in life and the frequency of attacks can vary from once or twice a year to every few days in the most severely affected patients, with nearly every patient being slightly different. These swellings can affect many areas of the body and usually last from 3 to 5 days, the types of attack are as follows;
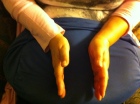
Localised subcutaneous swelling – affecting hands, feet, limbs, genital areas and trunk.
 Abdominal angioedema – symptoms include severe abdominal pain, nausea, vomiting and diarrhoea and abdominal distension. Because of large shifts in body fluids, symptoms of physical shock may be present. Many patients have received incorrect diagnosis, treatment and surgery for abdominal attacks in the past.
Abdominal angioedema – symptoms include severe abdominal pain, nausea, vomiting and diarrhoea and abdominal distension. Because of large shifts in body fluids, symptoms of physical shock may be present. Many patients have received incorrect diagnosis, treatment and surgery for abdominal attacks in the past.
Laryngeal oedema – Facial or lip swelling may progress to affect the larynx. If untreated swelling of the airway (larynx) may result in death from asphyxiation. Voice changes and difficulty in breathing are very serious symptoms. It is very important that swelling of the face and airway are treated as soon as symptoms occur
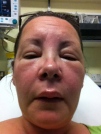
Don’t I look wonderful ! Facial swelling Sept 2011
 Some patients can identify warning symptoms (Prodomal symptoms) in the 24 hours before an attack. These symptoms can include extreme tiredness, a rash or tingling over the affected site
Some patients can identify warning symptoms (Prodomal symptoms) in the 24 hours before an attack. These symptoms can include extreme tiredness, a rash or tingling over the affected site
An example of a HAE rash from HAE UK website.

There are some things that are known to make a HAE patient more vulnerable to an attack of swelling. I don’t get the rash and rarely get any warning but in my case I know that hormones, stress & infection are my main triggers, and it’s usually a combination of things that trigger a major attack. Some other known triggers are
- Minor trauma e.g. repetitive daily activities when gardening, or in the gym.
- H.pylori (a bacteria that can be present in the stomach).
- Dental treatment – swelling typically occurs about 6 hours after treatment.
- Intubation when having a general anaesthetic.
- Surgery
- Drugs – ACE inhibitors, oestrogen in the contraceptive pill or in hormone replacement therapy.
Like many other people suffering with rare long term conditions, I consider myself to be a patient expert, qualified by my own research and the daily experience of living with HAE. Whilst I try my best to stay positive and keep healthy, these attacks can come on from nothing to acute in a matter of minutes, which has a vast impact on the quality of my life.
My first attacks occurred when I was 3 years old which were mainly face, hands or feet swellings and continued randomly throughout my childhood. I also had frequent stomach aches, diarrhoea and vomiting but no one linked the symptoms , and all allergy testing drew a blank. I felt I was just seen as a sickly child who often missed school. In my early teens when puberty hit I also had to deal with the break up of my parents marriage, and my condition worsened. I had frequent acute stomach attacks, often passing out with the pain. I know I had a reputation of being an attention seeking neurotic, and remeber several occasions when I was told it was all in my head. I was taken to many different hospitals & clinics for various tests and was finally diagnosed in July 1976, aged 15, by the wonderful, and very caring, Immunologist Dr Rita Brown at The Royal Berkshire Hospital (RBH) in Reading . It was a massive relief, although back then the conditions was referred to as Hereditary Angioneuroticoedema (HANO), which didn’t help with many health care professionals attitude!
I was started on the normal prophylactic treatment which was, and still is, Tranexamic Acid tablets daily. After years of taking these regularly, playing with the dosage and keeping diaries I don’t think it makes any difference to the number or severity of my attacks. Alternative treatments are steroid based Danazol or Stanozolol but again they have had limited efficacy and although I did try them in my twenties I had a significant number of side effects when taking them for any length of time ( I turn into something like a Tazmanian Devil as my poor long suffering husband can confirm).
From diagnosis through to my early 20s I had regular attacks that co-incided with my menstrual cycle. The pain was so acute that I was hospitalised several times a year, often via ambulance, and usually ended up spending at least 3 days in hospital, far more if the attack happened on a Friday or over the weekend , with my longest hospital stay being 9 days! Back then the treatment for acute attacks was Fresh Frozen Plasma and pain relief. Things did settle down a bit in my late 20’s until my pregnancy , then everything went very wrong for me. I was admitted to hospital several times up to 20 weeks and then stayed in hospital permanently for the last 4 months, but that is a story for another blog!
After having my daughter, in May 1992 , my attacks improved for about 5 years . Up to this point I had been treated locally at RBH, but when Dr Brown retired they closed the immunology department and I was transferred to the John Radcliffe Hospital in Oxford, a 45 minute trip each way on a good day!
It was around this time that Berinert was prescribed to me as a named patient for the first time. I still had to present at RBH A & E and wait for the drug to be authorised, usually after a phone call to an immunologist at JRH. Once prescribed it had to be found from Pharmacy, or on one occassion another hospital, and administered. However, once I was given a dose I was usually out of hospital within 2 days possibly 3. This was a massive improvement and things improved even further when I was allowed to keep my own supply at home, enabling quick administration as soon as I arrived at A & E, though this did depend completely on the doctor I saw on admission. It is only prescribed for use in acute abdominal attacks or those above the neck, as it is a very expensive treatment (my current dosage is 3 vials at a total cost of approx £2,800) and I occasionally need two doses to get an acute attack under control. However all the research, anecdotal evidence from fellow sufferers and my own experience shows that early administration improves efficacy, reduces the need for a second dose and significantly reduces length of an attack.
Attacks can build slowly or can come on in a matter of minutes so over the next ten years I got more practice at knowing when to take myself to hospital. It is a very personal decision and involves balancing the need for quick, in many cases life saving treatment against all the other considerations of presenting at A & E with a rare condition. i.e. Travelling to hospital 25 minutes away in extreme pain, will the flag still be on my record or will it have disappeared meaning delays before being triaged and the increased uncertainty of how quickly I might get treated, the understandable but very frustrating ” lets just rule out other pain causes” route taken by A & E staff with no experience of HAE , the vagueries of night & weekend shift staffing, the risk of being admitted to avoid overstay of the 4 hour target , the awful feelings of guilt that I’m adding pressure to already overstretched staff.
My husband has by necessity also become an expert ! He is able to explain the condition very calmly, can advise how best to mix up the drug so it dissolves fully, ready for injection. He has saved me from many delays by firmly pointing out that “yes he is sure this is an HAE attack, so please just give the C1 so we can avoid any risk of asphyxiation!” I also built up a file of documents to take with me, first those provided by the now defunct PIA (Primary Immunodeficiency Association) then documentation developed by the JRH Immunology and more recently the wonderful patient association HAE UK. However, even if I don’t encounter any problems getting treated it is nearly always a draining experience, not least as I have dreadful veins. After years of blood tests, canulas and injections they are very scarred and it often takes two attempts for the professionals to site a canula, as my veins just run away from the needle. So for a few years I preferred to stay home and take opiate pain relief rather that face the added stress that a trip to A&E entails. However that all changed in 2009 when I had my first laryngeal oedma, requiring a very dramatic blue light ambulance ride from my GP, and since then I have had a 3 further emergency throat swellings. So now I always attend A & E for all swellings above my neck. My records show that I haven’t treated a stomach attack in the last three years, though I know I have had at least 2 major episodes each year. Sometimes this means spending a day or two in bed but it also means that an attack usually takes longer to fully resolve , and untreated attacks can last for 5 to 7 days and subsequent localised/rebound swellings often occur.
Over the years I have missed work regularly, which has caused extra stress, and have lost count of the family & social occassions I have missed out on and the money I have lost in deposits or tickets never used! However, over my lifetime the majority of my attacks have been mild, and for large periods of my life they have been infrequent, so I know that I am lucky. I didn’t fully appreciate this until 2011 when found the help and support of two wonderful women Ann Price & Rachel Annals who run the amazing patient association HAE UK (check out their website http://www.haeuk.org). I now get support from the website and from their secure Facebook page. In November 2011, at the age of 50 , I finally had my first meeting with another HAE sufferer, when I attended their patient conference in Manchester. I can honestly say it changed my life. To finally be able to discuss this very complex condition and know that someone understood was a massive weight off my shoulders. I was able to explain my concerns about self administration, which I had finally been offered this year due to the increase in my attacks, and it was through their advise and support that I have finally gained the confidence to accept the training. For the last month I have been very excited at the prospect, because it gives me real hope that I will gain a degree of control over the severity and length of my Hereditary Angioedema attacks, which should improve the quality of my life and I’ll be less reliant on the amazing NHS A&E services. Whilst I don’t relish being my own personal pin cushion I have no fear of needles and I’m not worried about the thought of actually injecting a needle into my skin. However sitting here now I’m also quite scared as I’m deeply concerned about the emotional effects it will have if
a) the training brings on an attack.
b) I do pass the training –
i) how I will have to deal with the difficulties of how replacement of the Berinert will be managed across Trust boundaries ? There are already issues now when trying to get a replacement prescription as I leave A&E, which causes a strange and
unhealthy mix of frustration & self justification, with associated feelings of anger & guilt. I can see that this will be far
harder when I have to hold a bigger stock for repeat prescriptions, especially if I treat all acute attacks.
ii) will it change my relationship with my consultant if my usage does go up
dramatically?
iii) will I actually being able to repeat the process one handed whilst in pain? Not something that can be
replicated in training, knowing how darn difficult the professions find it with two hands!
c) I don’t pass the training – my disappointment and feelings of failure could exacerbate my condition in the short term and
I will have to continue to balance the need for treatment with the anguish of going to A & E.
These thoughts have been building up and causing me sleepless nights all week, but somehow typing them out has put them back into perspective. So instead I’m going to concentrate on all the positives
1) The cost savings at only having to attend A & E if I have a throat swelling.
2) The expected reduction in the number of acute attacks by promptly treating all acute attacks.
3) A reduction in the duration of attacks.
4) Regaining some control of my own health.
5) A massive improvement to my quality of life.
So I must finish off now and get this published so I can get a good nights sleep, and dream of nice juicy veins all eager and ready to provide perfect target practice. Wish me luck !







 Abdominal angioedema – symptoms include severe abdominal pain, nausea, vomiting and diarrhoea and abdominal distension. Because of large shifts in body fluids, symptoms of physical shock may be present. Many patients have received incorrect diagnosis, treatment and surgery for abdominal attacks in the past.
Abdominal angioedema – symptoms include severe abdominal pain, nausea, vomiting and diarrhoea and abdominal distension. Because of large shifts in body fluids, symptoms of physical shock may be present. Many patients have received incorrect diagnosis, treatment and surgery for abdominal attacks in the past.